
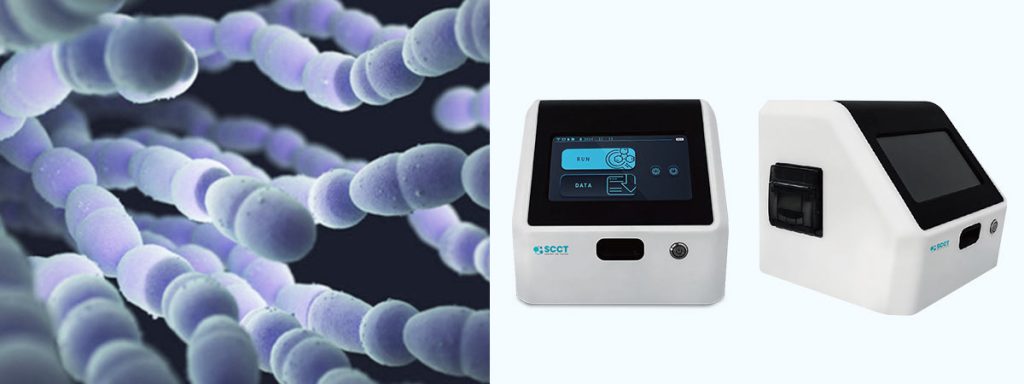
Mycoplasma presents a challenge in dairy herds because it lacks a cell wall. This unique feature prevents antibiotics like β-lactams and glycopeptides from working. Farmers often see increased somatic cell count and reduced milk yield when mastitis occurs. Monitoring infection with a somatic cell count tester helps track udder health and recovery. Practical mastitis screening supports early detection and better herd management.
| Condition | Somatic Cell Count (SCC) | Milk Yield (l) |
|---|---|---|
| Mycoplasma Co-infection | 550.3 | 29.0 |
| Conventional Pathogens | 389.3 | 29.9 |
| Non-infected Cows | 67.3 | 34.4 |
Key Takeaways
- Mycoplasma bacteria lack a cell wall, making standard antibiotics like beta-lactams ineffective.
- Regular monitoring of somatic cell count (SCC) helps detect mastitis early and supports better herd management.
- Using a somatic cell count tester provides quick results, aiding in timely decisions for cow health.
- Implementing frequent mastitis screening can significantly reduce infection rates in dairy herds.
- Veterinarians should guide antibiotic choices based on culture results to ensure effective treatment against Mycoplasma.
Mycoplasma and Antibiotic Resistance
No Cell Wall, No Beta-Lactam Effect
Mycoplasma bacteria stand out because they do not have a cell wall. This feature places them in the Mollicutes class. Most antibiotics, such as penicillins and cephalosporins, work by attacking the bacterial cell wall. Without this structure, these drugs cannot harm Mycoplasma. The table below highlights this resistance mechanism:
| Evidence | Description |
|---|---|
| Lack of Cell Wall | Mycoplasma, belonging to the Mollicutes class, do not possess cell walls. |
| Resistance Mechanism | Beta-lactam antibiotics target bacterial cell walls, making them ineffective against Mycoplasma. |
Note: All mycoplasmas lack a cell wall, which results in inherent resistance to beta-lactam antibiotics such as penicillin.
Why Standard Antibiotics Fail?
Antibiotics that target the cell wall, including beta-lactams (penicillins, cephalosporins, carbapenems, monobactams) and glycopeptides, do not work against Mycoplasma. These drugs bind to proteins involved in cell wall synthesis. Since Mycoplasma lacks this target, the antibiotics have no effect. Other common antibiotics, such as streptomycin and gentamycin, also show limited or no activity against Mycoplasma. This resistance means that standard treatments for mastitis often fail when Mycoplasma is the cause.
- Mycoplasma bacteria lack a cell wall.
- Antibiotics that target the cell wall are ineffective.
- Beta-lactam antibiotics (penicillins, cephalosporins, carbapenems, monobactams) are ineffective.
- Glycopeptide antibiotics are also ineffective.
- Penicillin has no effect on Mycoplasma.
- Streptomycin and gentamycin are generally ineffective.
Biofilms and Evolving Resistance
Mycoplasma can form biofilms, which are protective layers that shield bacteria from antibiotics. These biofilms make it harder for drugs to reach and kill the bacteria. When researchers disrupt these biofilms, antibiotics like doxycycline, levofloxacin, and erythromycin become more effective. The table below shows how biofilm disruption lowers the growth of Mycoplasma:
| Antibiotic | Biofilm Condition | Growth Index Comparison |
|---|---|---|
| Doxycycline | Disrupted | Significantly lower |
| Levofloxacin | Disrupted | Significantly lower |
| Erythromycin | Disrupted | Significantly lower |
Genetic mutations also play a role in antibiotic resistance. Changes in certain genes, such as the 23S rRNA gene, can make Mycoplasma less sensitive to macrolides and other drugs. Mutations in topoisomerase and DNA gyrase genes lead to resistance against fluoroquinolones. Some strains show increased expression of ABC-type genes, which pump antibiotics out of the cell and create multidrug resistance.
- Mutations in the 23S rRNA gene decrease susceptibility to pleuromutilins and macrolides.
- Changes in topoisomerase IV and DNA gyrase genes cause resistance to fluoroquinolones.
- Increased ABC-type gene expression leads to multidrug resistance.
Tip: Biofilms and genetic mutations make Mycoplasma infections harder to treat and require careful antibiotic selection.
SCC and Mastitis Screening in Mycoplasma Infections
SCC As an Infection Marker
Somatic cell count serves as a reliable indicator of infection and recovery in dairy cows. When a cow develops mastitis, the SCC rises as the immune system responds to the invading bacteria. Mycoplasma infections often cause a moderate increase in SCC, while environmental mastitis pathogens can trigger much higher levels. The following table shows how SCC changes during different infections:
| Infection Type | SCC Range (cells/mL) | Duration (days) | Clinical Symptoms |
|---|---|---|---|
| Mycoplasma arginini | 0.5 × 10^6 to 0.8 × 10^6 | 5 | Transient increase, no severe symptoms |
| Streptococcus dysgalactiae | 1.60 × 10^6 to 2.11 × 10^6 | 10 | Severe clinical symptoms |
| Rechallenge with Streptococcus dysgalactiae | 5.00 × 10^6 to 21.5 × 10^6 | > 28 | Severe clinical mastitis |
A cow’s SCC may return to normal after recovery, but persistent elevation signals ongoing infection or reinfection. Monitoring SCC helps farmers detect mastitis early and track the effectiveness of treatment.
Tip: Regular SCC monitoring allows for early intervention and supports udder health.
Using a Somatic Cell Count Tester
Farmers use a somatic cell count tester to measure SCC quickly and efficiently. This device provides immediate results, helping them make informed decisions about individual cow culture and herd management. Although SCC testing offers valuable information, studies show that it is not sensitive enough for herd-level surveillance of mycoplasma mastitis. Molecular methods, such as real-time PCR, detect mycoplasma infections more accurately than traditional culture methods.
| Evidence Type | Description |
|---|---|
| Sensitivity of SCC | Recent studies indicate that SCC is not sensitive enough for herd-level surveillance of Mycoplasma mastitis. |
| Comparison with Molecular Methods | Molecular methods, such as real-time PCR, are more sensitive than traditional culture methods for detecting Mycoplasma-related mastitis. |
Farmers often combine SCC testing with individual cow culture to identify infected animals. This approach improves the accuracy of screening and supports targeted treatment. The somatic cell count tester remains a practical tool for routine monitoring, especially when paired with other screening methods.
Note: Combining SCC testing with molecular screening increases the likelihood of early detection.
Mastitis Screening for Early Detection
Mastitis screening plays a crucial role in maintaining herd health. Early screening reduces the incidence of mycoplasma mastitis and improves outcomes for affected cows. Farms that implement early screening programs see a drop in mastitis cases, with rates decreasing from 2.8 percent to 0.5 percent. This improvement highlights the importance of timely intervention.
Screening frequency matters. Monthly or quarterly bulk tank cultures help detect mycoplasma early. Increasing the frequency of testing enhances the chances of finding infections before they spread. Farmers should follow these steps for effective screening:
- Weekly composite string sampling and culturing of all cows in positive strings until all cows test negative.
- Weekly mycoplasma bulk tank culture for at least four months after the last positive culture.
- Ongoing monitoring of all fresh cows, heifers, and clinical cows after a herd experiences mycoplasma mastitis.
- Bulk tank testing for mycoplasma at least once a month.
- Routine culture of all new additions, fresh cows, and heifers to provide early warning of infection.
Callout: Early mastitis screening and regular SCC checks protect udder health and prevent outbreaks.
Farmers who use individual cow culture and frequent screening can identify infected cows quickly. This approach limits the spread of infection and supports long-term herd health. Screening remains the foundation of mastitis control, especially when paired with SCC management and somatic cell count tester use.
Treatment Choices and Udder Health
Effective Antibiotics for Mycoplasma
Veterinarians often recommend macrolides, tetracyclines, and fluoroquinolones for clinical mastitis caused by Mycoplasma. These intramammary antibiotics target the bacteria’s protein synthesis or DNA replication, which helps control the pathogen. Unlike beta-lactams, these drugs can reach the site of infection and act on the bacteria. However, farmers must consider possible side effects when using these treatments:
- These drugs may cause adverse effects on the liver and kidneys, such as hepatitis or cholestasis.
- Dysbiosis can occur, leading to gastrointestinal infections and antibiotic-associated diarrhea.
- Residues in milk may affect both treated animals and humans, impacting milk quality.
Veterinarians should always base antibiotic therapy on culture results and sensitivity testing. This approach ensures that the chosen intramammary antibiotics will work against the specific pathogen present in the herd.
SCC Trends During Recovery
High somatic cell counts often signal ongoing clinical mastitis. Farmers use SCC trends to monitor the effectiveness of treatment and the recovery process. A steady decline in SCC after starting intramammary antibiotics suggests that the therapy is working and the pathogen load is decreasing. If SCC remains high, the infection may persist, or the pathogen may resist the current treatment. Regular bulk tank culture and individual cow culture help track these trends and guide further decisions.
Tip: Monitoring SCC and bulk tank culture results helps maintain milk quality and supports early detection of contagious mastitis.
Protecting Udder Health Long-Term
Long-term udder health depends on more than just treating clinical mastitis. Farmers should follow several strategies to prevent recurrence and protect milk quality:
- Dry-cow management, including teat dipping and dry cow therapy, reduces infection rates.
- Therapy during lactation, guided by a veterinarian, ensures proper treatment for clinical mastitis.
- Culling cows with chronic infections limits the spread of pathogens.
- Keeping the herd closed, testing new cattle during quarantine, and controlling farm traffic all help prevent new introductions of Mycoplasma.
- Using foot baths and disinfectants for visitors protects the herd from outside pathogens.
- Developing a vaccination program with a veterinarian adds another layer of defense.
Routine bulk tank culture and SCC management remain essential for early detection of clinical mastitis and for maintaining milk quality. These practices, combined with targeted intramammary antibiotics and strict biosecurity, help control the spread of pathogens and support long-term udder health.
Conclusion
Standard antibiotics fail against Mycoplasma for several reasons:
- These bacteria lack cell walls, so drugs like beta-lactams and glycopeptides do not work.
- Mycoplasma shows increasing resistance to macrolides and fluoroquinolones.
- Unique genetic adaptations and variable surface proteins help Mycoplasma evade treatment.
Regular SCC monitoring and mastitis screening help detect infections early. The somatic cell count tester, such as the California Mastitis Test, supports quick identification and management. Farms should keep bedding clean, train staff on milking protocols, and track progress monthly.
For best results, they should consult veterinarians for tailored prevention and treatment strategies.
FAQ
What Makes Mycoplasma Mastitis Different in Dairy Cows?
Mycoplasma mastitis in dairy cows stands out because the bacteria lack a cell wall. This feature makes standard antibiotics ineffective. Dairy farmers often see persistent infections. Early detection and targeted treatment help protect dairy herd health.
How Can Dairy Farmers Detect Mycoplasma Infections Early?
Dairy farmers use regular somatic cell count testing and pcr methods for early detection. pcr identifies Mycoplasma DNA in milk samples. This approach allows dairy producers to act quickly and prevent the spread of infection in the dairy herd.
Why Do Standard Antibiotics Fail in Dairy Herds with Mycoplasma?
Standard antibiotics target bacterial cell walls. Mycoplasma bacteria in dairy herds do not have cell walls. This resistance means dairy producers must use alternative antibiotics. Dairy veterinarians recommend drugs that target protein synthesis or DNA replication.
What Role Does Pcr Play in Dairy Herd Management?
pcr offers high sensitivity for detecting Mycoplasma in dairy herds. Dairy producers rely on pcr to confirm infections when somatic cell counts rise. This tool supports accurate diagnosis and helps dairy veterinarians choose the best treatment for the dairy herd.
How Can Dairy Farms Prevent Recurring Mycoplasma Outbreaks?
Dairy farms prevent recurring outbreaks by practicing strict biosecurity, regular pcr screening, and culling chronically infected cows. Dairy staff should follow hygiene protocols. Routine monitoring and early diagnosis protect the dairy herd and maintain milk quality.